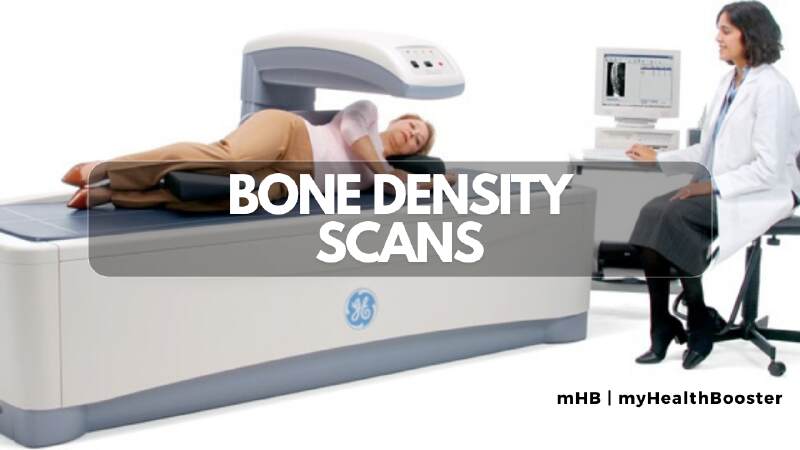
Key Points about Bone Density Scans
- Osteopenia, or low bone density, affects about 40% of postmenopausal women in the U.S., with an additional 7% experiencing osteoporosis, significantly increasing the risk of fractures.
- One in three women and one in five men over 50 may suffer bone fractures related to osteoporosis, emphasizing the importance of early detection through bone density scans.
- About 33% of people with hip fractures face dependency or nursing home care within a year, underscoring the need for timely detection and suitable therapy.
- Bone mineral density (BMD) estimation is crucial, particularly for women aged 50 to 65 with osteoporosis risk factors and all women over 65, as well as men and women on certain medications or with specific health conditions.
What is Osteoporosis?
- Osteoporosis is characterized by bones that are less dense and, consequently, less robust, increasing the risk of fractures even with minor traumas.
- It affects an estimated 44 million Americans, with 10 million having osteoporosis and 34 million having lower-than-normal bone mass (osteopenia), putting them at higher risk of developing osteoporosis.
- Women are four times more likely to develop osteoporosis than men, with risk factors including age, family history, stature, lifestyle, smoking, alcohol, and certain medications.
How Osteoporosis Occurs
- Osteoporosis results from an imbalance between osteoclast and osteoblast activity, influenced by various factors such as disease, hormonal changes, aging, menopause, and inadequate calcium and vitamin D intake.
- Thinning of bones occurs due to increased resorption by osteoclasts compared to bone deposition by osteoblasts.
- Cancellous bone is affected more rapidly than cortical bone, especially in areas with a higher ratio of cancellous to cortical bone, such as the spine, wrist, and hips.
What is Bone Mineral Density (BMD)?
- BMD, measured through a DXA scan, correlates with bone strength and the ability to bear weight, aiding in predicting fracture risk.
- BMD testing cannot guarantee the certainty of developing a fracture but helps assess the risk.
- It is distinct from a bone scan, which detects tumors and infections, and is crucial in diagnosing osteopenia and osteoporosis.
Who Should Have BMD Testing?
- BMD testing is recommended for all women over 65 and postmenopausal women under 65 with risk factors. Men and women with specific risk factors should discuss testing with their healthcare professional.
- Risk factors include a personal or family history of fracture, low body weight, smoking, corticosteroid use, impaired vision, and other health conditions.
How BMD is Measured?
- DXA is the preferred method, involving low-dose X-rays, quick and painless, with minimal radiation exposure.
- Results, reported as T-scores, help categorize bone density as normal, osteopenic, or osteoporotic.
- DXA reports include the test date, location, equipment details, reason for the test, diagnosis, results at tested sites, comparison with prior tests, fracture risk estimate, vertebral fracture assessment, and recommendations for follow-up.
The Importance of BMD Measurement
- BMD helps assess the risk of osteoporosis-related fractures, guiding optimal treatment decisions.
- It is crucial in determining the need for nonprescription or prescription medication therapy to reduce fracture risk.
- For those with fractures or planning orthopedic surgery, a diagnosis of osteoporosis influences surgical planning and treatment strategies for better outcomes.
What are other methods of measuring BMD?
There are small DXA scanners called peripheral DXA machines. These machines often measure BMD at the heel (calcaneus), shin bone (distal tibia), or kneecap (patella). Regular DXA machines have a standard reference (called NHANES III) that can be used for all machines, no matter the manufacturer. However, peripheral DXA machines do not yet have a uniform reference standard for the normal peak young adult bone mass that can apply to all machines and all manufacturers. This is necessary for peripheral DXA to be ready for more widespread use. Efforts are in progress to make the peripheral DXA technique more standardized. At present, it is best used as a screening test to consider whether or not a patient would benefit from further bone density testing.
Quantitative computed tomography (QCT) can be used to assess BMD. A standard CT scanner is used in this method. However, the amount of radiation exposure is higher than with DXA and the cost is greater. For these reasons, QCT is not in general clinical use.
Ultrasound is a relatively new diagnostic tool to measure BMD. There is no radiation source with this procedure. An ultrasound beam is directed at the area being analyzed. The scattering and absorption of the waves allow for an assessment of bone density. The results are not as precise as with the other methods mentioned. This technique is relatively new, and there is considerable research being conducted in this area. Since ultrasounds can easily be performed in a physician’s office, this method may become valuable for screening larger populations if its accuracy becomes more refined. If the BMD is low on the ultrasound test, you might be asked to have a DXA scan to confirm the results.
New techniques that are being developed to measure both the BMD and even the quality of the bone are micro CT and MR, which use technologies related to CT and MRI scans. These are not yet available for clinical use.
How often should DXA scans be repeated to monitor treatment?
The frequency of monitoring osteoporosis treatment using DXA scans is highly controversial. Some health care professionals recommend DXA scanning at one- to two-year intervals to monitor changes in bone density during treatment. But recent scientific evidence questions the usefulness of such interval monitoring. Reasons why repeating bone density scans is extremely tricky include:
Bone density changes so slowly that the changes may be smaller than the measurement error of the machine. In other words, repeat DXA scans cannot distinguish between a “real” increase in bone density or a mere variation in measurement from the machine itself. Typically, BMD changes 1% per year, which is less than the error of a DXA machine (usually in the range of 3%). Changes of less than 2%-4% in the vertebrae and 3%-6% at the hip from test to test can be due to the precision error of the method.
Whereas the real purpose of prescription osteoporosis treatment is to decrease future bone fractures, there is no good correlation between increases in bone density as measured by DXA with decreases in fracture risks with treatment. There are multiple examples of this in recent clinical studies. For example, the improvement in BMD only accounted for 4% of the reduction in spine fracture risk with raloxifene (Evista), 16% of the reduction in spine fracture risk with alendronate (Fosamax), and 18% of the reduction in spine fracture risk with risedronate (Actonel, Atelvia). Thus, improvement in BMD does not indicate the amount of the antifracture benefit of osteoporosis medication. Prescription medication may decrease a person’s risk of fracture even when there is no apparent increase in BMD. Physicians and nonphysicians alike are often surprised to learn this information!
Even if the DXA scan shows continued deterioration in bone density during treatment, no research data exists demonstrating that changing a medication, combining medications, or increasing medication doses will be safe and helpful in decreasing the future risk of fractures compared to just continuing the same medication.
Even if a person’s bone density deteriorates during treatment, it is quite likely that the person would have lost even more bone density without treatment.
What is the cost of DXA?
The cost for DXA scanning varies depending on insurance policies and coverage. In general, a patient without health care coverage paying cash can expect to pay approximately $200-$300 U.S. for the procedure.
What about the accuracy of BMD testing in the doctor’s office using smaller equipment?
There are several devices that are smaller than the standard DXA scanners that are being used in health care professional’s offices to screen for low bone density. Very little scientific data is available about these smaller units. Most of the information comes directly from the equipment manufacturers themselves. Many of these models test peripheral bones in the feet or hands. Other units use ultrasonography. These techniques can be less accurate than BMD testing performed with state of the art equipment. Additionally, office-testing equipment can range dramatically in price and quality.
In general, these devices may be reasonable to measure overall fracture risk but are not useful in monitoring therapy. Their use might be limited to screening and results would require confirmation using DXA. In addition, expertise in using the equipment and interpreting the data can vary. At present, it is difficult to comment on these other methods of BMD testing. Interpretation of the results of these tests may be more difficult and not as reliable as the standard DXA scan. Some doctors use these as screening tools and recommend more formal DXA testing if they are abnormal.
Summary
Osteoporosis is a disease that results in a significant risk of fracture. The consequences of fracture can include hospitalization, immobility, a decrease in the quality of life, and even death.
From a larger perspective, it is a costly disease in terms of the health-care system and time lost from work. Early detection and therapy is the mainstay for trying to prevent these complications. BMD testing results correlate well with the risk of fracture, and the testing is easily performed in a time-efficient manner without any discomfort. Although many methods of BMD testing exist, the best currently is DXA scanning. It is imperative that testing ultimately be done using state-of-the-art equipment with capable highly trained personnel and a doctor well versed in interpreting the results.